Understanding Pregnancy Tumors
Categories: Health
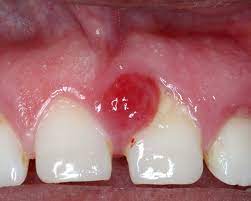
Pregnancy Tumors:
Tumours give this illness a far more serious seeming name than it actually is. Up to 5% of pregnant women experience pregnancy tumours, which are benign tumours that do not spread malignancy. Pregnancy tumours are often elevated, distinct nodules that range in size from 0.5 to 2.5 centimetres. While some women experience pain from them, others do not.
Although the exact cause of pregnancy tumours is unknown, it is believed that variations in hormone levels are a contributing factor. As was stated above, taking proper care of your teeth and gums throughout pregnancy is crucial. Gingivitis and poor oral hygiene increase your risk of developing pregnancy tumours.
Bring it to your dentist's attention if you do spot what you believe to be a pregnancy tumour on your gums. They can certify that there is nothing more sinister than the tumour. After giving birth, many pregnancy tumours naturally disappear, but if yours persist or are uncomfortable, you can have them removed—likely with a laser or cryosurgery.
Pregnancy tumours are benign growths that can appear during pregnancy. They are often referred to as pyogenic granulomas or granuloma gravidarum. Despite not having cancer, they can still be uncomfortable and need medical attention.
Here is a quick summary of their causes and available treatments:
Causes:
Hormonal changes: Pregnancy tumours can form as a result of changes in hormone levels, particularly higher amounts of oestrogen. Vascular and connective tissue growths have been connected to oestrogen.
Local irritation or trauma: Pregnancy tumours can develop in the oral cavity as a result of chronic gum irritation or trauma, such as poor oral hygiene, gum disease, or accident.
Treatment options:
Observation: After birth, some pregnancy tumours may naturally regress. A "wait and watch" strategy may be used if the tumour is tiny and not causing much pain.
Good oral hygiene: By regularly brushing and flossing your teeth, you can lower your risk of difficulties and help stop the growth of pregnancy tumours.
Professional cleaning: The treatment of pregnancy tumours may benefit from a dentist's scaling and cleaning of the teeth and gums. Plaque, bacteria, and other irritants that promote their growth are removed through this process.
Surgical removal: Surgical intervention may be necessary for pregnancy tumours that are larger or more persistent. In order to reduce any potential hazards to the foetus, this treatment is normally carried either after the first trimester or after birth.
When pregnant, do tumours grow more quickly?
Most of the time, being pregnant won't accelerate the growth of cancer in your body. Hormone alterations can occasionally promote particular tumours, such as melanoma, but this seldom happens. Most of the time, cancer won't harm your unborn child, but some treatments could be dangerous.
Can a tumour stop ovulation?
The uterus (womb) or ovaries may get compressed by a tumour or another issue, which would impair their functionality. Egg release, fertilisation, or implantation are all prevented by damage to other reproductive system components.
During pregnancy, cancer diagnosis:
Pregnancy is characterised by a variety of symptoms, including nausea, vomiting, abdominal bloating, breast alterations (lumps), rectal bleeding, exhaustion, and headaches. But occasionally a particular cancer type can also be linked to these symptoms. If symptoms persist or occur at a stage of the pregnancy when it is no longer thought to be normal, it is crucial to discuss them with your doctor.
Cancer may occasionally be discovered during pregnancy before it would have been otherwise. For instance, a standard Pap test performed during pregnancy can detect cervical cancer. Ovarian cancer may be discovered during a pregnancy ultrasound.
You could be concerned about harming the unborn child if tests are used to diagnose cancer if it is suspected. You might be concerned about the radiation exposure from x-rays, CT scans, or nuclear medicine studies, for instance. However, some of these tests are safe to use while expecting, giving your doctor additional knowledge to help treat the malignancy.
Which tumours are prevalent during pregnancy?
The most frequent malignant tumours during pregnancy are those of the breast, cervix, and ovary. Pregnancy does not, however, seem to have an impact on the overall prognosis and survival rates for these tumours according to stage. During the planning stages of treatment, ethical, emotional, and therapeutic difficulties could arise.
Is a tumour dangerous while pregnant?
Breast, cervical, lymphoma, and melanoma cancers are the most prevalent types of cancer during pregnancy. Rarely does cancer itself cause birth defects, and some cancer treatments are safe to use while pregnant. Together, your healthcare practitioner and you will search for the best course of action.
Although they are uncommon, pregnancy-related tumours can occur. The two types of tumours are benign and malignant. Unwanted growths are not cancer. cancerous ones are. Breast, cervical, lymphoma, and melanoma cancers are the most prevalent types of cancer during pregnancy. Rarely does cancer itself cause birth defects, and some cancer treatments are safe to use while pregnant. Together, your healthcare practitioner and you will search for the best course of action. Your options will depend on the type, size, and stage of your cancer as well as how far along the pregnancy is.
Gestational trophoblastic disease (GTD) is a different type of tumour that can affect women. When a fertilised egg fails not develop into a foetus, it occurs. Finding GTD is not always simple. Although most of it is benign, some varieties can be cancerous. A pregnancy of the molars is the most prevalent form of GTD. It may first resemble a typical pregnancy. If you experience vaginal bleeding—not monthly bleeding—you should visit your doctor.
The sort of tumour, whether it has spread to other areas, and your general health will all influence how it is treated.
If you think you could have a pregnancy tumour or other oral health issues while pregnant, it's crucial to speak with a healthcare provider like a dentist or obstetrician. Based on your unique situation, they can offer a precise diagnosis and suggest the best course of therapy.